MI-TLIF — minimally invasive stabilization
The current gold standard is open TLIF — a reliable, classical technique proven over decades. MI-TLIF developed as a less invasive variant: instead of detaching the muscles, we work through them with percutaneous screws. Clinical results are similar, but the patient experience is significantly better.
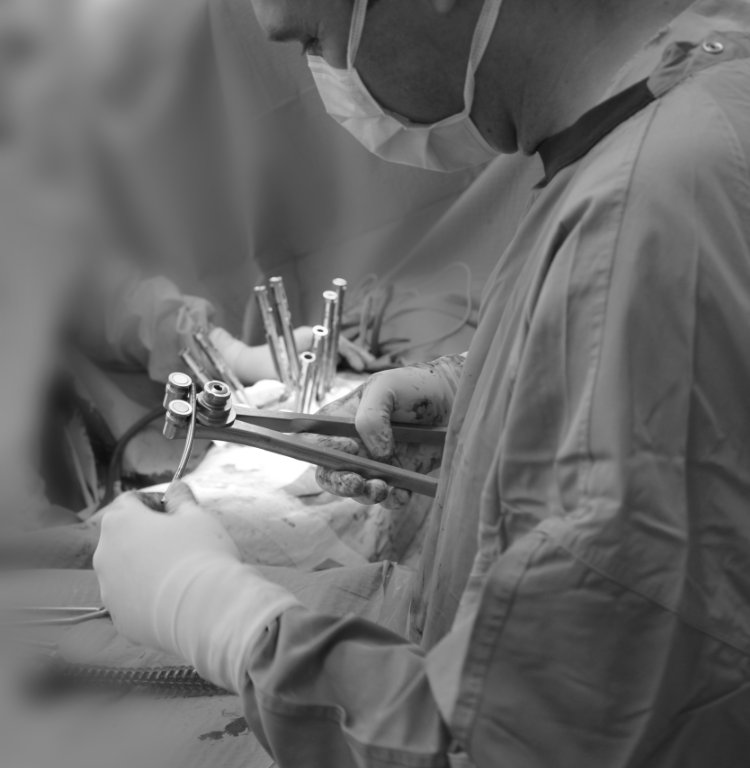
The essence of the technique: percutaneous titanium screws are placed into the pedicles of the vertebrae through small skin incisions, under imaging guidance. Between two adjacent screws, a tube (tubular retractor) is advanced down to the spine, splitting the muscle fibres apart — not detaching them. Through this corridor, the damaged disc is removed and a cage filled with bone-graft substitute is placed. The screws are connected with rods, securing stability.
Muscle preservation
Muscle fibres are not detached from the bone — they are split apart. The function of the surrounding musculature is better preserved, which is particularly advantageous for younger, active patients.
Less blood loss
Minimal exposure and targeted work significantly reduce intraoperative blood loss compared to the open technique.
Shorter hospital stay
Faster mobilization and less postoperative pain typically translate into a shorter hospital stay.
Faster recovery
Muscle preservation and reduced tissue trauma allow a faster return to everyday activity, with less postoperative muscle pain.
Note: MI-TLIF is technically more demanding than classical open TLIF — which is why fewer surgeons perform it routinely. Beyond the long learning curve, it requires specialised imaging equipment and instrumentation. This is the technique in which I have built the deepest experience over the years, and for younger patients I typically choose this approach.
