Precisely where the source of pain is
One of the most effective tools in non-surgical spine care is the CT-guided targeted block injection. Imaging guidance ensures that a minimal amount of medication is delivered exactly where the source of pain is, without unnecessarily burdening the rest of the body.
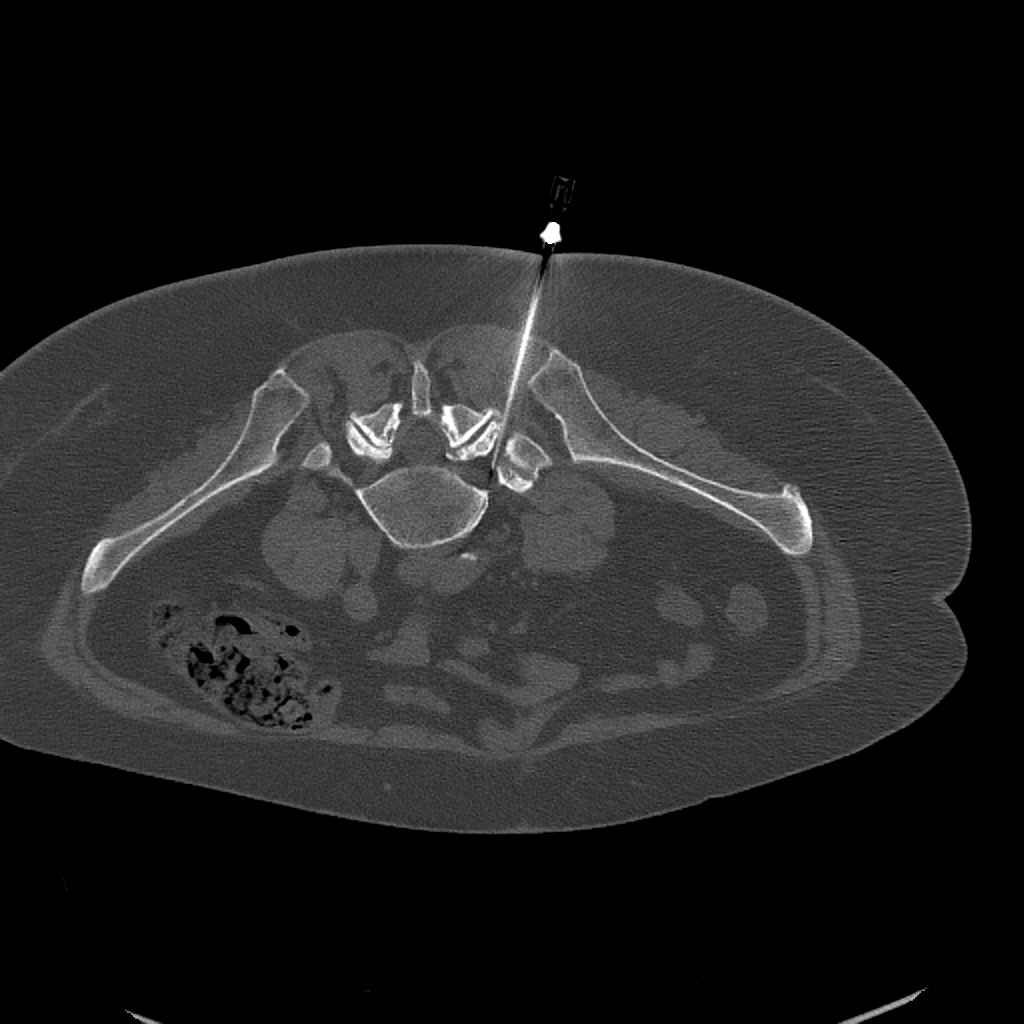
Nerve root block
If the nerve emerging between the vertebrae is the source of pain — for example due to compression from a disc herniation or spinal stenosis — a targeted nerve root block is the appropriate intervention. During the procedure, a minimal amount of local anaesthetic and anti-inflammatory steroid is delivered next to the affected nerve root.
Needle placement is verified using CT or fluoroscopy, so that the treatment reaches only the inflamed nerve. The local anaesthetic may cause temporary numbness or weakness — this is a normal phenomenon that typically resolves within a few hours.
Facet joint block
Increased loading of the small joints between the vertebrae (facet joints) accelerates cartilage wear (arthrosis), which can produce mechanical-type low back pain that worsens with movement. In such cases, a small amount of local anaesthetic and anti-inflammatory steroid is delivered into the painful joint, again under CT or fluoroscopic guidance.
How the procedure works
- Diagnosis confirmed by imaging (MRI) is required
- Needle position is verified using CT or fluoroscopy
- A 10–30 minute observation period is required after the procedure. A recovery bed is available if needed.
- If symptoms have resolved, the patient can go home unaccompanied
- Driving on the day of the procedure is not recommended
Contraindications · special caution
- Hypersensitivity to any of the agents used
- Anticoagulant (blood thinner) use requires coordination: with acetylsalicylic acid (e.g. Aspirin) the block can proceed; with clopidogrel a 7-day pause is recommended, with other anticoagulants a 2–5 day pause
- Uncontrolled blood sugar or hypertension — the treating physician must be informed
- Active infection at the treatment site or systemic infection
